Our program focuses on the core knowledge, skills, and understanding of the following topics:
- Allergy and immunology, anatomy and embryology, genetics, microbiology, pathophysiology, pharmacology, endocrinology, and neurology as they relate to the head and neck
- Basic sciences as relevant to the head and neck and the upper aerodigestive system
- Communication sciences, including audiology, speech and language pathology and the voice sciences as they relate to laryngology
The educational program also includes the clinical aspects of diagnosis and the medical and surgical therapy for diseases, neoplasms, deformities, disorders and injuries of the ears, the upper respiratory and upper alimentary systems, the face, the jaws, and other head and neck systems.
Following completion of the educational program, residents should be prepared to serve as a comprehensive otolaryngologist:
- Care for patients of all ages with medical and surgical disorders of the ears, the upper aerodigestive system and related structures of the head and neck
- Carry out diagnostic evaluations of patients with otolaryngologic disorders
- Carry out the surgical and nonsurgical management of otolaryngologic disorders, including rehabilitation and referral to subspecialists when appropriate
As a vital adjunct to the acquisition of the required medical knowledge and patient care skills, the resident will acquire the skills needed to practice medicine in a complex medical system. The interpersonal and communication skills needed for such a practice as well as expertise in systems-based practice are continually emphasized and evaluated throughout the residency. Proper professional behavior is fostered as the resident masters the essential skills of practice-based learning that will prepare him or her for a lifetime of learning.
Research
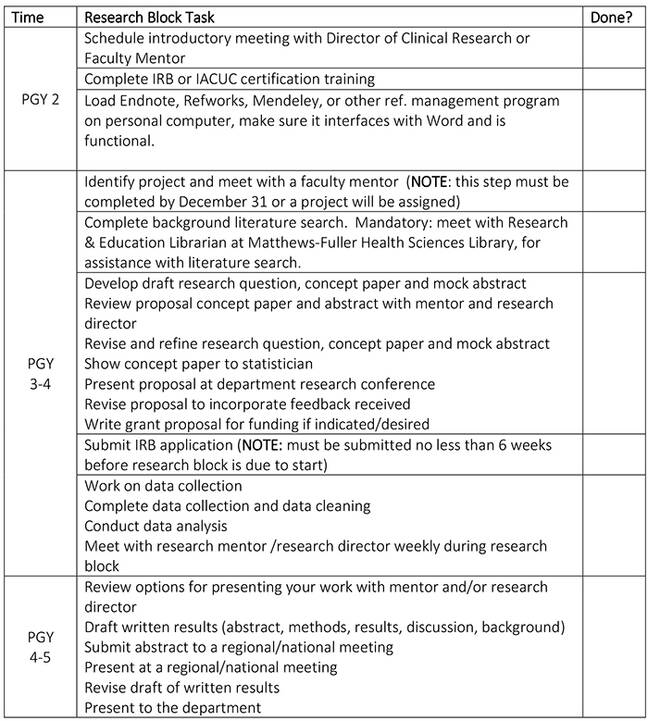
The resident's research experience is well structured and closely monitored.
Faculty research summaries
James Saunders
Dr. Saunders has broad research interests and have completed many research projects on the etiology and treatment of hearing loss in low resource environments, particularly in Nicaragua. This work includes projects: evaluating the cost-effectiveness of hearing loss interventions such as cochlear implants in low resource countries throughout the world, exploring innovative technologies for large scale hearing screening, investigating the genetic causes of hearing loss in Nicaragua, and studying the role of environmental toxins (e.g., heavy metals and pesticides) on pediatric hearing loss in low resource settings. Working with the Dartmouth Space Medicine Innovations Lab, he is developing novel ways of detecting central auditory processing impairments through tablet-based screening and evoked potentials. He is also involved with multiple projects to investigate the role of bacterial resistance on treatment outcomes in chronic otitis media and to develop novel surgical techniques in chronic ear surgery. He also serves on the Lancet Commission for Hearing Loss, which is generating a detailed report on global hearing loss, and on the Otolaryngology – Head and Neck Surgery Global Initiative, an international research consortium. He serves on the Steering Committee for the World Hearing Forum at the World Health Organization. He is a co-founder of the Coalition for Global Hearing Health, an international organization to promote hearing healthcare in low resource environments, and of Mayflower Medical Outreach, an organization that supports and trains otolaryngologists and audiology providers in Nicaragua.
Joseph Paydarfar
Dr. Paydarfar’ s research is focused on improving outcomes in head and neck surgery, capitalizing on the strong collaborative ties Dartmouth Hitchcock Medical Center has with the Dartmouth Thayer School of Engineering. We currently have active projects investigating optical imaging to improve margin control in oral cavity resections, image guided surgical navigation to improve safety and efficacy of transoral robotic surgery, and surgical simulation tools for training and research purposes. Residents and medical students involved in our research have enjoyed a close working relationship with engineering students and learn various technical skills such as computer aided design and 3D printing.
Ryan Little
Dr. Little’s research interests focus on innovative approaches to studying sinonasal and olfactory disease, combining microbiome and immunologic science with emerging technologies to improve understanding of disease mechanisms and patient outcomes. As a fellowship-trained rhinologist and skull base surgeon, he serves as the Director of the Sinus Research Center, working closely with DartCF, the Dartmouth Cystic Fibrosis Research Center, to study sinonasal disease in CF and non-CF populations via interdisciplinary translational research. This work includes ongoing investigations of host–microbiome interactions and sinonasal inflammation in patients with cystic fibrosis, including a foundation and center-supported study evaluating the impact of CFTR-modulator therapy on sinonasal microbial communities, inflammation and olfaction. He also pursues novel imaging strategies to characterize the olfactory cleft and better define olfactory neuroepithelium pathology, collaborating with colleagues in neurosurgery. In addition, Dr. Little leads clinical trials of biologic therapies and drug-eluting implants for chronic rhinosinusitis, and remains deeply committed to resident education, directing the Advanced Sinus & Endoscopic Skull Base Dissection Course and mentoring trainees in research and clinical development. Dr. Little serves on committees for both the American Rhinologic Society and the American Academy of Otolaryngology — Head & Neck Surgery.
Eric Holmgren
Dr. Holmgren’s research mainly focuses on maxillofacial trauma particularly the biomechanics of the fractured or repaired mandible. He works closely with the Thayer School of Engineering in order to model and clinically test the mandible. Currently his research is concentrated on the mandibular angle fracture and the effects of patient-specific morphology and a plate selection guide. Also, he is working on a study evaluating patient perception regarding timing of facial fracture repair. Other recent published works have focused on maxillofacial case reports and a study looking at anatomical predisposition to the mandibular angle fracture.
Louise Davies
Dr. Davies has appointments in both the Department of Surgery and with The Dartmouth Institute for Health Policy and Clinical Practice. She is senior faculty of the VA Outcomes Group, a long-standing multidisciplinary research group at the White River Junction VA Medical Center, where she also serves as Chief of Otolaryngology. Her clinical practice focus areas are thyroid and parathyroid disease, cancers of the head and neck, and voice and swallowing disorders. She is an Associate Editor for JAMA Otolaryngology - Head and Neck Surgery, a former Fulbright Global Research Scholar, and in recognition of her cancer epidemiology research expertise has served on national and international task forces. Her methodologic research expertise is in cancer epidemiology, cancer screening, and the use of mixed methods research approaches for research on patient experience, healthcare delivery science and in clinical trials. Her current areas of funded research are 1) epidemiological modeling of thyroid cancer to understand the contribution of over diagnosis, possible new causes of disease, and the impacts of policy and guideline changes, 2) the development of informational calculators that give personalized estimates of prognosis for newly diagnosed oral cancer patients, 3) recruitment interventions to support surgical randomized trials, 4) measurement of excess mortality during the COVID pandemic due to disruptions in healthcare.
Eunice Chen
Dr. Chen has 2 main translational research interests that aim to improve head and neck cancer treatments and outcomes by (1) utilizing electron paramagnetic resonance (EPR) oximetry to measure tumor and tissue oxygen levels directly and (2) developing paired agent imaging to aid in fluorescence-guided margin assessment for squamous cell carcinomas of the head and neck. She collaborates with research groups at the Dartmouth Cancer Center and the Thayer School of Engineering. Her clinical research interests include pediatric head and neck tumors including vascular anomalies, congenital hearing loss, and SARS-CoV-2 immunological response in adenotonsillar tissue. She has been a member of the American Academy of Otolaryngology-Head and Neck Surgery Pediatric Otolaryngology Education Committee since 2012 and has served as editor for the Home Study Course-Pediatric Otolaryngology Section and moderator for the FLEX XCast on Management of T+A Failures.
Leadership Preventive Medicine Residency
The Leadership Preventive Medicine Residency is a unique program in quality improvement, leadership and population health for residents and fellows already training at Dartmouth Hitchcock Medical Center. This program allows residents and fellows to obtain the MPH degree from The Dartmouth Institute, lead a practicum focused on improving care, and be able to sit for boards in Preventive Medicine.